With the first baby boomers turning 65 in 2011, America’s older population is in the midst of unprecedented growth. From a little more than one in ten in 2010, individuals aged 65 and over will account for one in five United States residents by 2030, while the number of people aged 75 and over will account for one in eight by 2040, up from one in sixteen today.
The aging of the population has broad implications for our society, some of which include increased pressure on government spending, slowing labor force growth, and growing demands on families to assist aging parents and relatives. But there are also significant implications for housing markets, as the need for homes that are affordable, accessible, and located in proximity to social and commercial centers and public transportation will rise.
In our latest report, Housing America’s Older Adults, we assess the implications of a rapidly aging population on housing demand and conclude that by a variety of measures the existing housing stock is unprepared to meet the escalating need for affordability, accessibility, social connectivity, and supportive services. Consider:
- High housing costs force millions of low-income older adults to sacrifice spending on other necessities including food, undermining their health and well-being.
- Much of the nation’s housing inventory lacks basic accessibility features, preventing older adults with disabilities from living safely and comfortably in their homes.
- The nation’s transportation and pedestrian infrastructure is generally ill suited to those who cannot or choose not to drive, isolating older adults from friends and family.
- Disconnects between housing and the health care system put many older adults with disabilities or long-term care needs at risk of premature moves to nursing care “facilities.”
The public policy challenges are immense. It is vital to our national standard of living that all levels of government recognize the implications of this profound demographic shift and take immediate steps to address these deficiencies. The private and nonprofit sectors also have critical roles to play in developing new housing and care options that support aging in community. It is also important that older adults and their loved ones consider how their housing needs and preferences are likely to evolve as they age and to take steps now to ensure that their homes and communities are able to support them in the years ahead.
Profile of an Aging Population
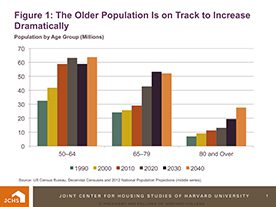
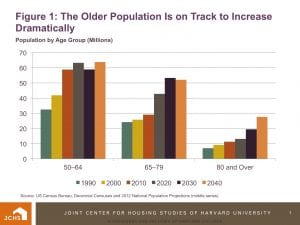
The older adult population has grown tremendously since the first of the baby boomers (born between 1946 and 1964) turned 50 in the mid-1990s. Between 1990 and 2010, the number of people of at least that age jumped by 35 million, an increase of 55 percent. Today, more than 63 million households—over half of the U.S. total—are headed by someone in their 50s or older.
With the oldest baby boomers reaching retirement age after 2010, the population aged 65 and over is projected to reach 73 million by 2030, an increase of 33 million in just two decades. By 2040, aging baby boomers will push up the population aged 80 and over to 28 million, more than three times the number in 2000.
The older population will also become more diverse as the wave of young immigrants who arrived in the United States in recent decades reaches age 50, prompting significant shifts in housing demand given the different housing situations and financial circumstances of people of color. For example, older Asians and Hispanics are more likely than whites or blacks to live in multigenerational households, and their rising numbers will therefore affect not only the demand for institutional care, but also the housing, financial, and personal situations of their family members. As a group, people of color also have lower rates of homeownership, lower median incomes, and fewer assets, all of which affect their housing options.
In addition, assuming the income distribution of the 50-and-over age group remains the same as it is today, there will be a substantial rise in the number of low-income households over the coming years. In 2024, 6.5 million older households will have incomes under $15,000—a jump of 1.8 million, or 37 percent, in a single decade. The number of older households with incomes between $15,000 and $29,999 will grow by 2.9 million. These statistics assume the income distribution of younger baby boomers—people now in their 50s—will keep pace with current retirees, but in the aftermath of the Great Recession, the reality is that this group is much less financially secure than its predecessors. Their lower incomes, wealth, and homeownership rates will affect their ability to cover the costs of appropriate housing and/or long-term care in their retirement years.
With age, people are also increasingly likely to face disabilities that pose challenges to independent living. The numbers of older adults with physical, cognitive, and financial limitations will increase sharply over the coming decades, particularly once the first baby boomers reach 80 years old in 2026. The U.S. Department of Health and Human Services estimates that nearly 70 percent of people who reach the age of 65 will ultimately need some form of long-term care, adding to the pressures on financially stretched older adults.
The vast majority of older adults live in their own homes. Even among those with disabilities, 90 percent reside in private homes rather than nursing homes or other forms of congregate care; and when asked about preferences for the future, most agreed that they would prefer to “age in place.” In a 2010 survey of 1,600 people aged 45 and older, AARP found that 73 percent strongly agreed that they would like to stay in their current residences as long as possible, while 67 percent strongly agreed that they would like to remain in their communities as long as possible. Given that 60 percent of adults aged 80 or older have lived in their homes for at least 20 years and another 18 percent for at least 10 years, most are already aging in place.
Still, many seniors may opt to move in their older years. Household changes such as retirement, children moving from the home or adult children returning to it, disability, or the death of a spouse may give rise to new housing needs and preferences. New models of housing may entice baby boomers to make different decisions than their predecessors. The need to find more affordable housing may become a greater concern for those living on fixed incomes. But financial constraints may also prevent people from adapting to their changing circumstances. Indeed, 24 percent of respondents to a 2010 AARP survey expressed a preference to stay in their homes for as long as possible because they could not afford to move.
Challenge: Affordability
As the single largest expenditure in most household budgets, housing costs directly affect financial security. Today, a third of adults aged 50 and over—including 37 percent of those aged 80 and over—pay more than 30 percent of their income for housing that may or may not fit their needs. Among those 65 and over, about half of all renters and owners still paying off mortgages have at least moderate housing cost burdens—and of these, 30 percent of renters and 23 percent of owners with mortgages are severely burdened, spending more than half their incomes on housing.
Devoting a substantial share of their incomes to housing means older cost-burdened households are forced to scrimp on other critical needs. Severely cost-burdened households headed by a person aged 50 and over in the bottom expenditure quartile spend 43 percent less on food and 59 percent less on health care compared with otherwise similar households living in housing they can afford. Not surprisingly, severely cost-burdened households headed by a person aged 50 to 64 save significantly less for retirement.
Homeowners who have paid off their mortgages by the time they retire, however, are in a much more advantageous position. In addition to having lower housing costs, homeowners—even those who still carry mortgages—typically have considerably more wealth than renters, in the form of both home equity and non-housing assets. These resources can help support the expense of changing needs later in life, including long-term care. Even excluding home equity, 35 percent of homeowners aged 65 and over have enough wealth to cover median annual nursing home costs for more than four years. The median renter, in contrast, cannot afford even one month in a nursing home. Indeed, only 13 percent of renters could pay for nursing home care for more than two years, and just 7 percent could pay for more than four years.
Homeownership rates vary widely by race and ethnicity. Among adults aged 50 and over, 81 percent of whites own homes, compared with 58 percent of blacks, 62 percent of Hispanics, and 70 percent of Asians. As people of color make up a greater and greater share of the population, this disparity in homeownership rates implies that more and more older adults will be housing cost burdened and therefore have less wealth to tap into to meet their needs as they age. In addition, given that people in their 50s today confront a number of financial pressures, including higher rates of mortgage and non-housing debt, cost burdens may become even more widespread over time.
Challenge: Accessibility
Millions of older adults live in homes that lack accessibility features, such as no-step entryways, single-floor living, extra-wide doorways and halls, accessible electrical controls and switches, and lever-style door and faucet handles. In fact, the 2011 American Housing Survey reports that just 1 percent of U.S. housing units have all five of these universal design features. Roughly two in five housing units in the country have either none or only one of these features.
Because of regional differences in housing stock, homeowners in certain areas may be more likely to have to make major modifications to enable a household member with disabilities to remain at home. In the Northeast, for example, many homes are built on multiple levels, without a bedroom and bathroom on the first floor. Even so, the costs of extensive home renovations, such as adding a first-floor bath or a no-step entry, are generally lower than the cost of extended stays in assisted living or nursing care.
Challenge: Social Connection
The majority of older adults live in low-density suburban and non-metro areas where it is difficult to shop, access services, or visit family and friends without using a car. Yet among people in their 80s and beyond, nearly a quarter of individuals do not own a car. And, as a recent AARP survey revealed, about one in five respondents aged 50 and over occasionally or regularly missed activities because of limitations on their driving.
City dwellers have greater access to transit but are no less at risk of isolation if they are unable to leave their homes alone because of safety concerns, have trouble getting to local transit stops, or do not have friends and family nearby. While transit is an option for some, older adults use these services less often than other age groups—suggesting that public transportation may not meet their needs for convenience, safety, and affordability.
Challenge: Long-Term Care
For individuals with disabilities or chronic conditions, the ability to age in place depends on having access to long-term care in their homes or communities. While Medicaid and Medicare generally do not cover such costs, some state Medicaid Home and Community-Based Services (HCBS) waivers do. Some may even pay for the cost of home modifications to improve accessibility. But eligibility requirements for this support vary widely, and need outruns availability. For those who are not Medicaid-eligible or do not qualify for waivers, the costs of in-home care can be substantial.
At any given time, only about 2 percent of older adults reside in group-care settings. Even so, assisted living facilities, nursing homes, and hospices provide critical support for those recovering from acute medical episodes or at the end of life. According to the Department of Health and Human Services, 37 percent of those aged 65 and over will receive care in an institutional facility at some point in their lives, with an average stay of one year.
Given the high costs of care, most people rely on family for some or all of their care. Many of today’s caregivers are themselves over 50, caring for both children and parents. This dual role can raise financial and emotional burdens, as well as housing challenges, should they choose to move to be near a parent or live in a multigenerational setting. Housing that allows family to live in close proximity, such as accessory apartments, can provide housing for caregivers or for older adults seeking to live closer to children, making care coordination easier. New types of housing, such as units with two master bedrooms, can create more flexible situations as needs evolve; and accessible rental housing can allow households to sell their homes but remain in their communities near family.
The Way Forward
Given the widely varying circumstances of older adults, meeting their housing and housing-related needs requires a range of family and financial planning responses. Building savings, managing debt, and obtaining long-term care insurance are all important steps toward continued self-sufficiency. Thoughtful choices about where to live, the type of housing to occupy, or timing home modifications in advance of disabilities or chronic conditions make it more possible to age in place without compromising safety or social connections.
But many people in their 50s and 60s simply lack the resources to obtain appropriate housing and services as they age, and so it is critical that the public and private sectors take steps to ensure that housing and health care systems support appropriate and cost-effective options for vulnerable older adults as well as those with means, and that communities provide housing options, transportation, and services to meet the needs of their older populations.
A number of promising entrepreneurial approaches have already emerged in the realms of design, urban planning, health and wellness, social engagement, and finance. Numerous cities and states are advancing livability through housing, transportation, and walkability initiatives, as well as through ordinances to promote accessibility in private homes. Various nonprofit and public initiatives are demonstrating the benefits of linking housing with long-term care. The private sector is also developing new housing options, technologies, and services in recognition of the potential market for assisting older adults with aging in the community. A broader conversation, however, is essential to help spread these initiatives so that more can benefit from them.
Most importantly, federal efforts need to be expanded. In particular, rental assistance makes a crucial difference in quality of life for those able to secure subsidized housing. At their current scale, however, these programs reach only a fraction of older renters with low incomes and high housing costs. Additional funding for housing with supportive services is also essential, given the limited number of new units added in recent years and the need for reinvestment in much of the housing developments that do exist. In addition, changes to Medicare and Medicaid would enable better coordination of affordable, accessible housing with long-term care.
For their part, state and local governments can promote accessibility in both the home and built environments, as well as expansion of both housing and transportation options. For example, they can require that all new residential construction include certain accessibility features, and offer tax incentives and low-cost loans to help owners modify their homes to accommodate household members with disabilities. In addition, localities can change their zoning to support construction of accessory dwelling units (ADUs) and mixed-use developments that add housing within walking distance of services or transit.
Municipalities—particularly the growing number with large 50-and-over populations—need to ensure that a range of services are available to older adults, including social and volunteer opportunities; education programs centered on health, finance, and housing maintenance; adult day care and meals programs; and health and wellness services. Meanwhile, state Medicaid programs can reorient their funding to enable low-income seniors to age in the community rather than in institutional facilities, as many are doing through Home and Community-Based Services waivers. With better coordination, state and local government programs for older adults would not only save on costs but also provide better outcomes.
Within the private sector, the aging of American society provides vast opportunities to innovate in the areas of housing and supportive care, while substantial business opportunities exist in helping older adults modify their homes to suit evolving needs, delivering services at home, and developing new models of housing with services that promote independence and integrate residents with the larger community.
Significant challenges lie ahead in ensuring that America’s older adults are safely, affordably, and comfortably housed, in locations that support their health and independence. A concerted effort is needed at all levels of government, by philanthropy and the public and private sectors, and through the advocacy of older adults themselves. But if we act now, the potential is there for older adults to have a higher quality of life than ever before, and for communities to be increasingly livable and vibrant as a result.




Comments